To say this has been a very stressful week, would be a huge understatement.
So much is riding on this extubation, and it has definitely taken a toll on me.
Ever since we've been back to Edmonton, I have never called in a night to check
on Evanna, because I know she's just fine (plus I know they would call me if
there were any concerns). However, ever since Evanna has been extubated, I've
called at least twice every evening. My nerves are at an all time high, and I
just want this part to be over with.
The big problem we were experiencing, is if something were to happen and Evanna
gets extremely upset, they can't really sedate her too much, because that would
mean she would stop breathing. So there's a fine line between keeping her
comfortable and happy, and over sedating her to the point that she stops
breathing, they have to reintubate her, and we're back to square one and
proceeding with a tracheotomy.
Anyways, I'm going to go over what has happened over the past week, so bear
with me. I know I've already posted about her extubation on Facebook and
Instagram, but this blog is a true journal of this journey, and I want to
document everything fully, as I plan to print this sometime in the future.
So since my last post, we were able to decrease her PEEP to 6 on the
ventilator by Monday, which meant that a Tuesday extubation was a GO! Dr.
Aditia was extremely disappointed that he wasn't going to be the one to do it
because he was off to China first thing in the morning, meaning that Dr.
Ryerson got the honour of being the one to extubate Evanna (the intentivists
are incredibly competitive with each other - it's actually quite funny). Her
extubation happened to fall on Day 100 of us being in the ICU, and so I'm hoping
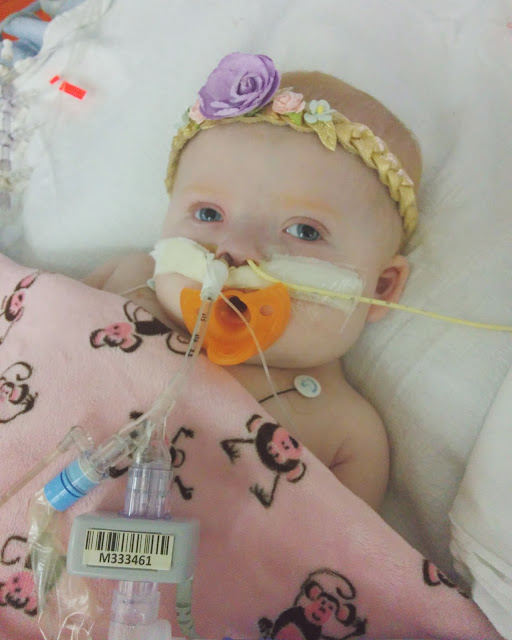
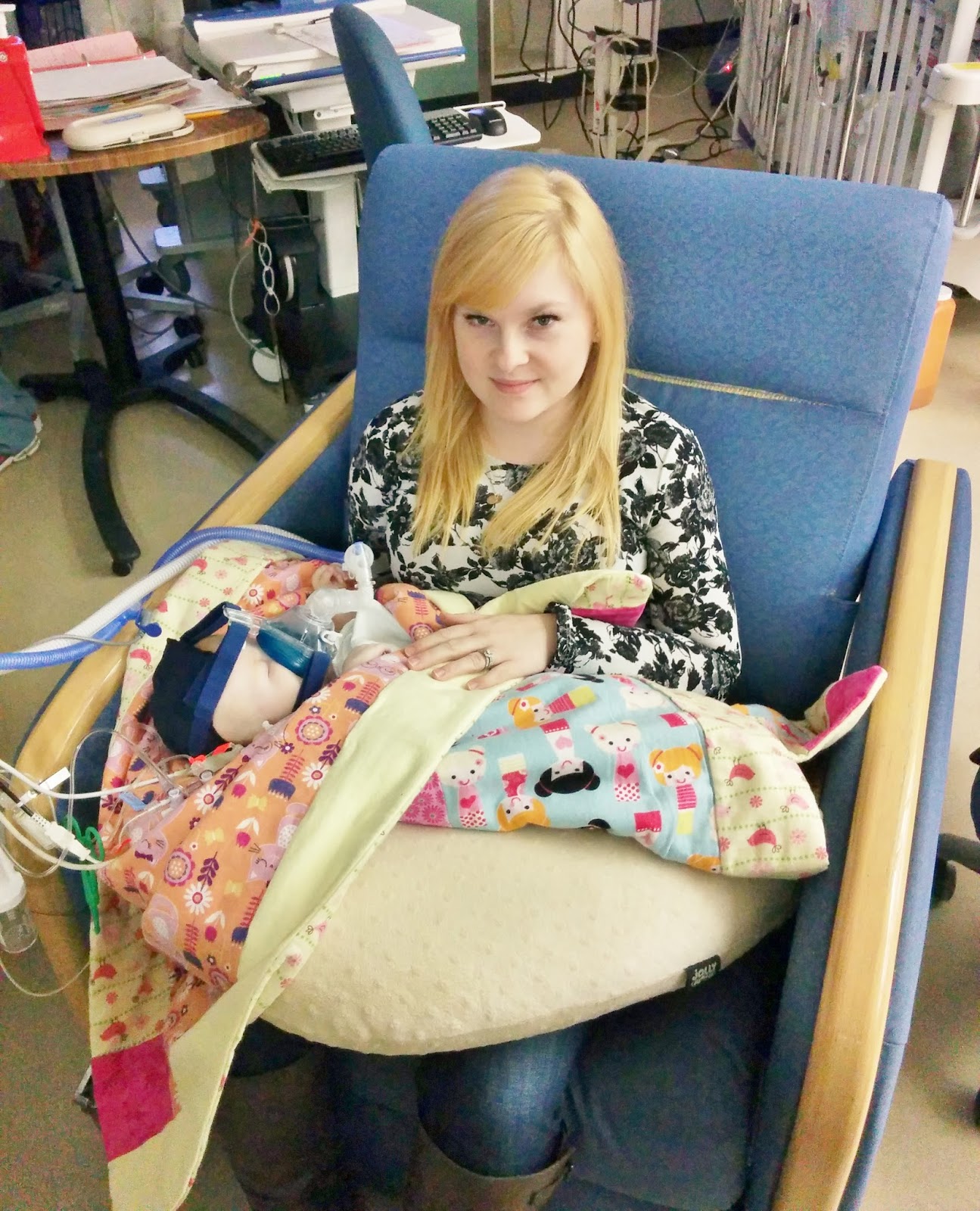
that means something. Like I expected, the extubation went smoothly, and I even
got to take a picture of her before they put the BiPAP mask on her. It was a
great day filled with so much hope and joy as we made this big step. Once
things were settled down, I even got to hold her, and according to my
calculations, it was the first time that I had held her in 44 days.
I came in on Wednesday, and Evanna had had a good night. The nurse asked if
I wanted to put an outfit on her, but I told her that when we were transferred
back up to Edmonton I hadn't bothered to bring any of Evanna's clothes this
time because I didn't think there was a point. So I raced over to West Edmonton
Mall and bought a few cute onesie’s from Carter's, and even found matching bows
at H&M while quickly shopping for myself. I came back and got her dressed
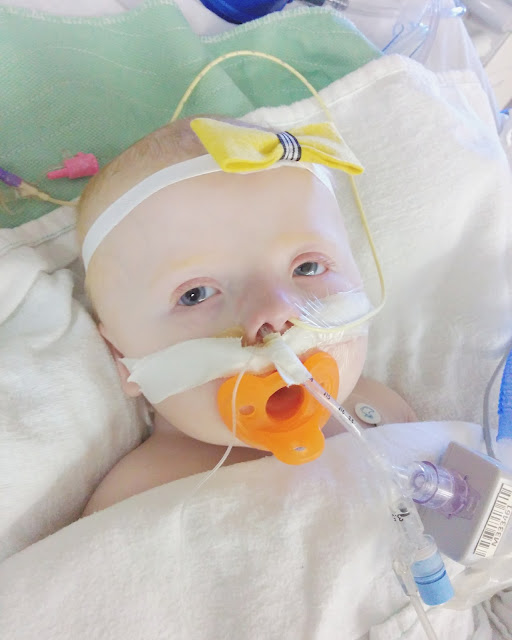
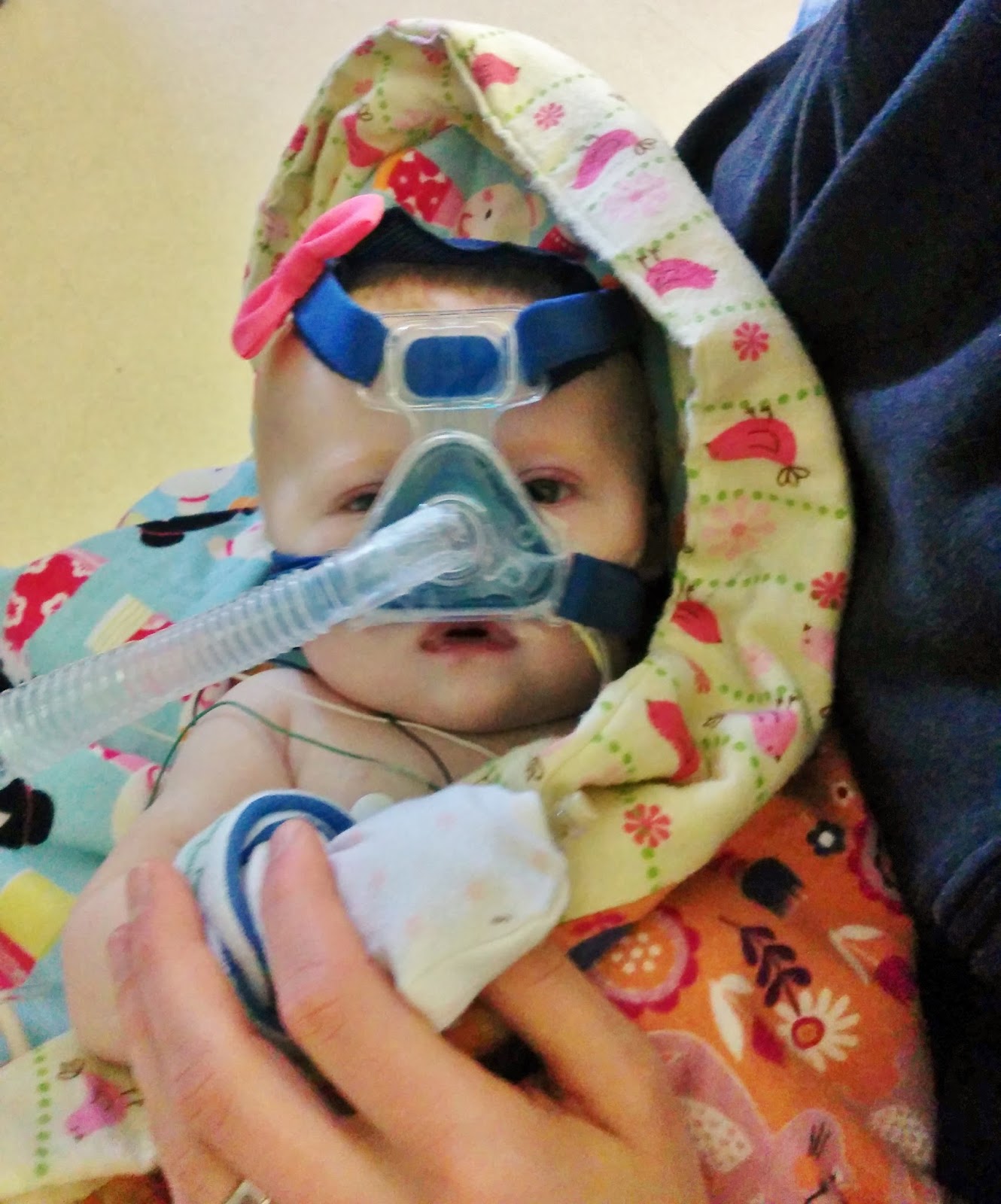
up, and decided to hold her again. That evening we tried her on nasal BiPAP,
but she didn't do as well as they thought she would, so they switched her back
to the full face mask. She also became really irritable that night, and so this
is when my stress levels started to climb, as she wasn’t doing as well as I had
hoped.
I came in on Thursday, and she was doing okay. Her evening was kind of
rough, but she had settled out and was doing much better. They switched her
ventilator settings to CPAP, but within a few hours her CO2 started to rise
again, so they went back to BiPAP settings and left her there. Dr. Ryerson
started to indicate that she was a little disappointed in the progress that
Evanna was making, and unsure of how this extubation was going to go. She
stated that she's not ready to give up on Evanna, but that I needed to know
that a tracheotomy may still be on the table as an option for her. That
evening, things just got worse. According to their calculations, they didn't
decrease her medications when they extubated her, but I felt that Evanna was
definitely experiencing withdrawals. Her heart rate went up to the 200s and
stayed like that for hours, she was flailing around and nothing I was did would
calm her down, her temperature was increased and she was tongue thrusting - all
signs of withdrawal. It takes a lot for me to freak out (I've seen Evanna code,
so I feel like I've practically seen it all), but I was truly going into panic
mode. I called Nick multiple times to keep him in the loop, and I was so close
to asking him to leave work and drive up to Edmonton as I felt she was about to
fail this extubation. Dr. Duff was our intentivist for the night, and he too
was worried that we were going to have to reintubate her again. He decided to
"throw the kitchen sink at her" (his words lol), and do everything
possible, just short of reintubating her, as he too didn't want Evanna to fail
this extubation. We upped her Milrinone (it's a drug that helps the heart
pump), drew cultures, started antibiotics, gave her fluid (a dry body can be
really hard on the heart), and upped her sedation doses. Finally around 11pm,
things started to settle down, so I finally left to get some sleep.
I called at 5am to check on her, and Dr. Duff answered the phone and said that
he hasn't had to touch her and for me to go back to bed and get some sleep.
Things settled a little bit on Friday, but my nerves were at an all time
high. Considering how things were going, I was terrified that Evanna was
failing this extubation. She had an incredibly good day with her O2 in the 80s
and her heart rate going as low as 140. They came back down on her Milrinone,
as well as some of her sedation. However, come evening, Evanna started to act
up a little bit (we're noticing a pattern here...), and was completely
miserable. It wasn't as bad as the previous night, but she was still a little
restless, and her heart rate went up again. They gave her some extra doses of
hydromorphine, which seemed to help, and I was told they had to do that a few
times throughout the night.
Evanna had a pretty good day yesterday, and I was so relieved to know that
Nick was on his way up to Edmonton. I was still really stressed and emotional
during rounds, so I was definitely in tears when Dr. Anand came by. I stated
that while I know Evanna isn't the number one priority on the unit, and there
are sicker kids than her here, that I need Evanna to be a priority for the next
week, as I really want this extubation to be successful. Dr. Anand assured me
that Evanna is a priority, and that he will definitely work with us to make
sure she is given the best chance possible to succeed. I definitely felt a lot
better after that, and I have since felt that my wishes are being met. We
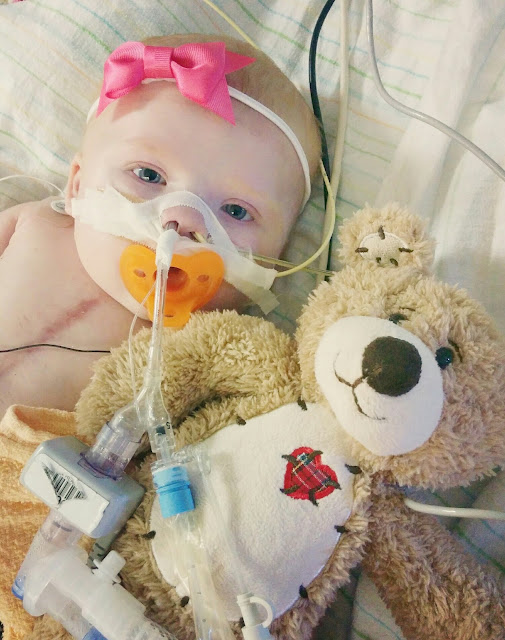
switched her to a nasal mask again, and though Evanna's CO2 levels initially
rose, we waited it out and they came back down. I also noticed that her
hemoglobin was low (I'm the first person to grab the blood gas results from the
RT’s and read them myself to see how Evanna is doing), and so I asked Dr. Anand
if we could think about doing a transfusion, as they always help boost her
energy and keep her sats higher (this is why blood donation is so incredibly
important!!). Dr. Anand agreed with me, and when I left to go pick Nick up,
they started a blood transfusion (what a little vampire!).
After I picked Nick up, we grabbed a quick bite to eat, and came back to the
hospital to see Evanna for a little bit. We didn't stay too long, as Nick had
just gotten off work himself that morning, but we waited until her 8 o'clock
blood gas to be done before we left (my life is currently revolving around
blood gas time - a sign we've been in the PCICU for too long lol).
Today has been a relatively good day. They finally turned off her Milrinone,
but that was it in regards to changes made for the day. She hasn't necessarily
been on it because of heart failure lately, but it was a drug they started when
we were back in Calgary (when she was experiencing heart failure), and because
she ended up being on it for a long time, it's something they've also had to
slowly wean. They left her ventilator settings alone, and if she has a good
night, they will hopefully do a small decrease tomorrow. On a positive note, Nick got to hold Evanna today, and again, according to my calculations, it's been 64 days since he last held her. He was one happy dad!

That's basically the story of our lives - slow and steady. We're still not out
of the woods in regards to the extubation, and I won't consider this a
successful extubation until we're on high flow. However, she is still extubated
(it's been longer than 4 days too), and still doing relatively well, so I’ll
take it. I'm scared that she's going to fail and she'll end up getting a
tracheotomy (not the worst thing in the world, but would still love to avoid
one), and I really just want to fast forward this part. Evanna hates the mask,
and this process has definitely been hard on me. I too hate the mask, and I
really hate all the unknowns of whether Evanna is going to succeed or not and
if we're doing this all for nothing.
Please continue to pray for our little girl, and that she will be comforted
during this not so pleasant part, and that she will continue to get stronger every
day and come off of the BiPAP and CPAP - and quickly too!
xo The Irvine Family