February 7-14 is
Congenital Heart Defect Awareness Week. To help raise awareness, spread
knowledge and share the effects of this disease, Jayme of The Paper Deer
Photography Blog, Christie of Lemon Squeezy Home and Kierra of The Irvine Home
are each sharing one story of a child with CHD every day to showcase the
trials, triumphs, journey and heartache of this devastating disease. We invite
you to read and share this project to further our voices. Thank you. #Facesof
CHD
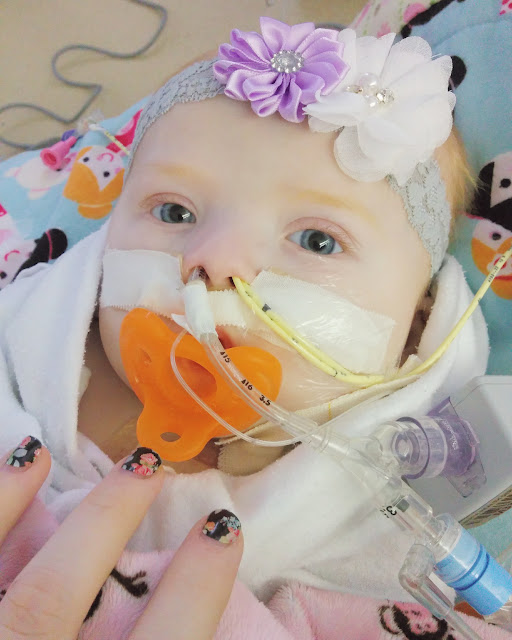
Meet Ava Monroe! Chandler and I (Kaila) have the privilege of
raising this extraordinary little, now 6 month old, life together. We live in Georgia, about 45 miles west of
Atlanta, and have been married for just shy of 3 years. After being diagnosed with PCOS several years
ago, we did not see a baby in our near future at all. Especially after being told we would need to
seek fertility to conceive. But just
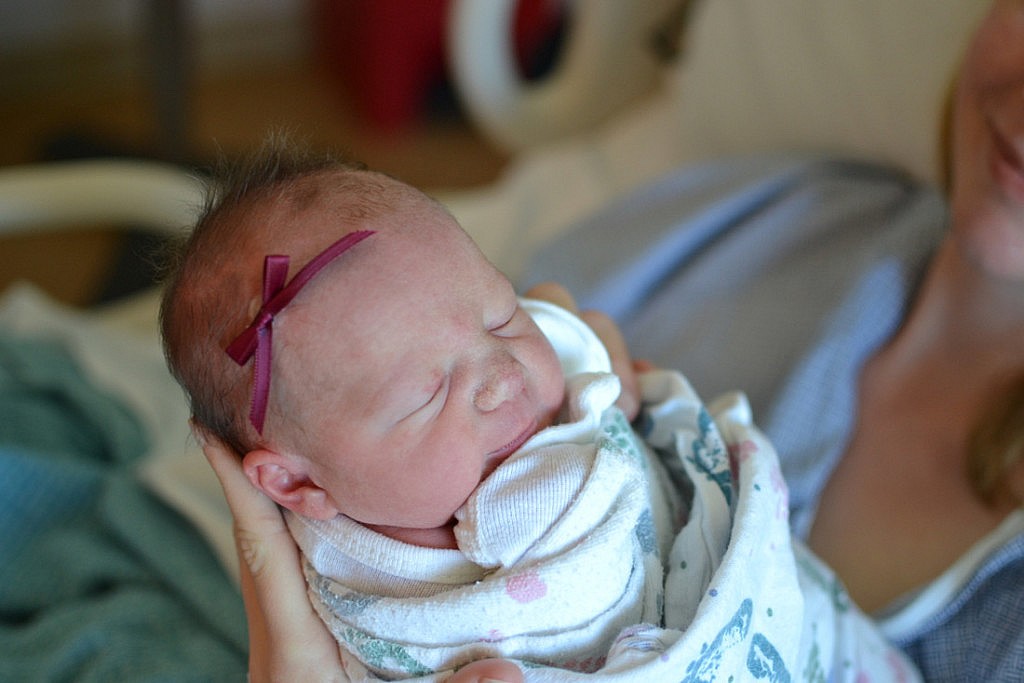
before Christmas 2013, we were shocked to find out that we would be welcoming
our little miracle in the summer.
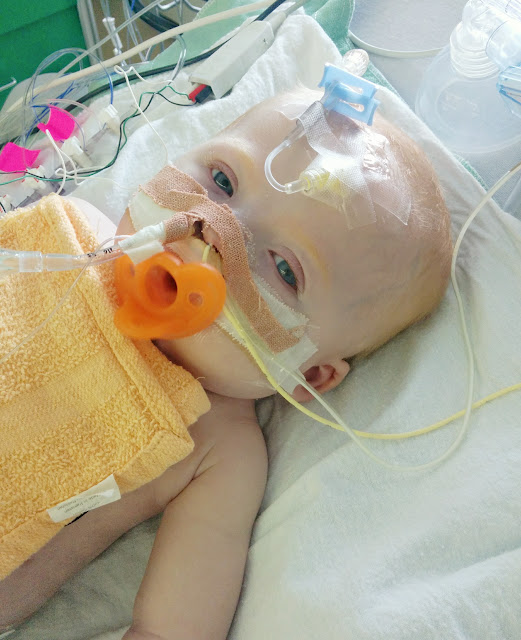
Ava’s journey in the CICU (Cardiac
Intensive Care Unit) began at just 12 hours old. Our brand new baby girl was transferred to
Egleston very quickly. And thanks to a
very easy delivery, I was discharged at the same time. This particular CICU was open-concept. There were 26 bed-spaces, and every last one
was full. This was seemingly nice for
the first… several hours. We met a few
parents, listened to their experiences and swapped pictures. But then, roughly 6 hours into our stay, the
baby in the bed space next to us lost his battle. My heart still drops as I replay the mother’s
screams in my head. They echoed through
the halls and into my soul. I remember
telling God, “do not let that be me”.
Other than surrounding chaos, our first
five days were full of optimism. The
week consisted of meeting with doctors & surgeons. They came up with her plan of care and
informed us that we were looking at 10-14 days of recovery before we would be
home-bound. Ava was not allowed food
that first week due to her specific CHD (Congenital Heart Defect) & required Prostaglandins to keep a special duct open until her surgery. She had no oxygen requirements, just IV’s
& central lines (which prevented us from holding her). On day 6, we walked alongside our baby girl
as they wheeled her back to the OR.
There was really no time to process any of it as we were immediately
dumped into a waiting room FULL of people, including much of our large
family. After hours of waiting, the
surgeon came and found us. He greeted us
with sweat dripping from his surgical cap.
Waiting for his words was the most nervous I had been up to that
point. He told us that he had repaired
Ava’s aortic arch and tried to get to her VSD but couldn’t cover it all. He went on to say that her pressures in her
right ventricle were “a little funky” and that he would watch that closely but
he hoped it would work itself out as her heart got accustomed to it’s new
“flow”. Thankfully, it did.
Nothing could have prepared for what we
walked in to. Just hours prior, we had
handed off our seemingly perfect, 5 lb, 14 oz. child. The sight that greeted us when we walked back
in to the CICU was simply terrifying.
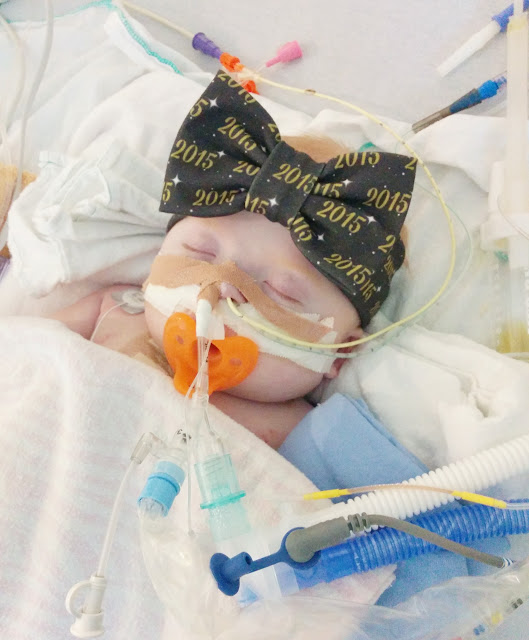
They had to leave Ava’s chest open
to allow room for swelling and extra fluid that had been pumped into her during
surgery. All that was covering her tiny
beating heart was a clear patch stitched between her chest bones. The nurses were whispering to us, assuring us
that she looked very good and letting us know we could touch her hands and
feet. They didn’t want us talking to her
too much or stimulating her, being that her little body had just experienced such
major trauma. It was all we could do to
text our families goodbyes. Truly, we
could not have faced anyone in those 4 days that she remained open. They were excruciatingly long. Once Ava was closed, they started lifting her
sedations relatively quickly. There was
such hope in seeing her big round eyes open after so long. I felt so disconnected from her, but so
admirable of her at the same time. I
just remember feeling like, we finally made it!
Our new life is about to start.
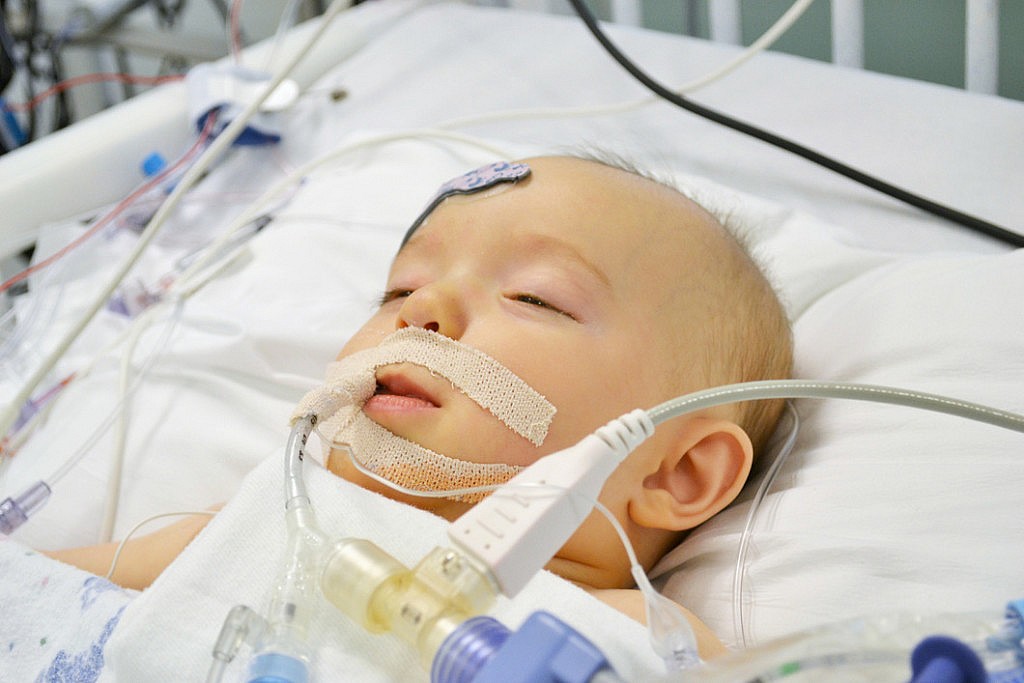
Two days later, they were ready to extubate
her (remove her breathing tube)! We were
anxiously awaiting this moment because this was a huge step toward going
home. As soon as they allowed us back in
the unit, there were nearly 10 people scrambling around Ava’s bed-side. They were already switching her from the
oxygen she was on to a RAM Cannula (which gives additional pressure to help
expand the lungs) and they assured us that it was very common for post-op
babies to need a little extra respiratory help immediately following a surgery
such as hers. However, within the hour,
it was clear that Ava’s respiratory status was declining and they emergently
re-intubated her. Little did we know, this
was the beginning of a new journey for us.

Ava’s first three extubations, were chalked
up to her just needing to regain strength. After all, time was not much to ask for after
what our girl had endured. So time we
gave her. After nearly a month since
surgery, it was time to extubate for the fourth time, things were going
surprisingly well. So well in fact, that
my mom came to sit with Ava while my husband and I made the hour+ drive home
for the first time. The second, and I
literally mean the second, that we
opened our front door.. I received a call from the CICU. The doctor was rambling and rambling and I
just remember screaming, “What Happened?!”. Ava had been re-intubated.. but that was not
all. She had a line that had been in her
right femoral artery for over 3 weeks. They
speculated that it must have formed a clot because after the nurse flushed her
line.. Ava lost all profusion to the lower half of her body. There was not adequate blood flow being
delivered to her lower extremities. We
immediately got in the car and headed back to Atlanta. My mom had been rushed out in the haste of
things. Ava was started on blood
thinners and they were hoping that things would resolve quickly. By the time we arrived, her left side looked
seemingly normal, but her right leg was very alarming. It was modeled, and there were spots of black and purple from her hip to her toes.
The lower you looked, the worse/darker it got. The vascular surgeons sent their best
ultrasound tech over to see what they could conclude. Our doctors seemed to be shocked by what had
happened, they said if this happened once a year that would be a lot. The vascular team could not locate the clot,
but informed us that it was not likely that our daughter would keep her right
leg. Devastated is too light a word. When you are battling such a devil as CHD,
and trying to make your mental list of things to prepare for, losing limbs is not
on that list.
The following days, despite what the
vascular doctor had expected, her leg continued to improve. And after a week, losing her leg had turned into, as the doctors put it, “JUST
losing her toe”. I remember dwelling on that word,
“just”. Many may have counted their
blessings at that point, but I was just so exhausted and so bitter. And after roughly a month and a half in the
hospital, nothing had gone right, nothing.
Once we got over that hump, we were back to the old grind of trying to
successfully extubate. But again, the
days were turning to weeks and every failed extubation turned into
another. Each time more devastating than
the last. Then, we had a terrible
scare. One morning, about a dozen
doctors were gathered around Ava’s bedside as we walked in. I had seen this before, around other babies,
and it was never good. They were all
looking at her x-ray. Some on their
phones with other doctors, some with pharmacy, others checking labs and
speculating amongst themselves. We had
seen her chest x-ray every single morning since we had been there. That being said, we noticed it
immediately: Her heart was doubled in
size. To any heart parent, this is a
nightmare, as it typically indicates heart failure. She had several close calls with cardiac
arrest and her heart began taking on the stress from all of her respiratory
troubles. Thankfully, with the help of
cardiac medication and another intubation, the stress on her heart slowly retreated.
But Ava was just pitiful. Her respiratory decline came quicker with
every extubation. I will never forget
hearing the whistle of air as she
fought for every unassisted breath. Her
violent retractions bore visibility to every centimeter of her ribs. My heart was breaking, and my faith, I would
have laughed at the very word. The
doctors did not think we would be bringing our daughter home, and although we
never spoke it to each other, my husband and I felt that dream slipping away.
During these horrible months, Ava had gone
to the OR several times for bronchoscopies to look at her airway. It was the same each time. She had suffered damage from the breathing
tube. But from what they could see,
nothing significant enough to be causing her respiratory failure. They then did an exploratory cath
procedure. But came back with nothing,
her lungs and pulmonary arteries were working well.
Every time we would check something off the
list, the more time had been wasted. All
the while, this tiny person was fighting for every breath and we were no closer
to offering her relief. The days were so
long, and the nights were longer.
Something as simple as gas pain was enough to send her over the edge,
and cause her to need to be emergently re-intubated. She had no energy left. My baby was aging, but not growing. I reached my limit of emotional, spiritual,
physical exhaustion and pain. I could
not watch her go on like this any longer.
I felt defeated. As I laid my
head on my precious daughter that night, I whispered to God, with a lump in my
throat, and a shattered heart, that he could have her back. Nothing in this life will ever be so painful. My husband and I sought nothing but each
others arms, we cried until we were shells of human beings. My husband told me that, as long as Ava
fought, we would fight with her. All it
took was one look to see that there was not much left in her tiny, beautiful
body.
That Wednesday, after a rough start to her
final attempt at kicking the breathing tube, Chandler demanded her to be re-intubated. We knew where it was headed and did not
desire to see her struggle, that intubation was simply a relief. From there, things moved quickly in the
direction of Ava getting a Tracheostomy and G-tube. It was the only way we would have a chance at
taking her home, and to relieve her of her burden. Within 48 hours, she had already had the
surgeries. And for the first time, in
over 3 months, things were looking up.
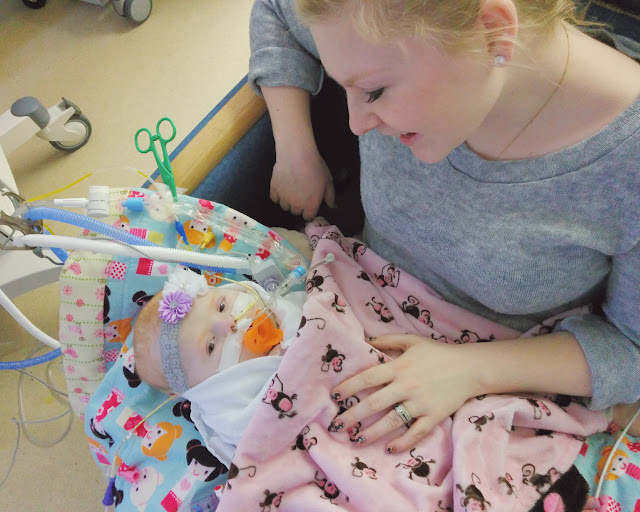
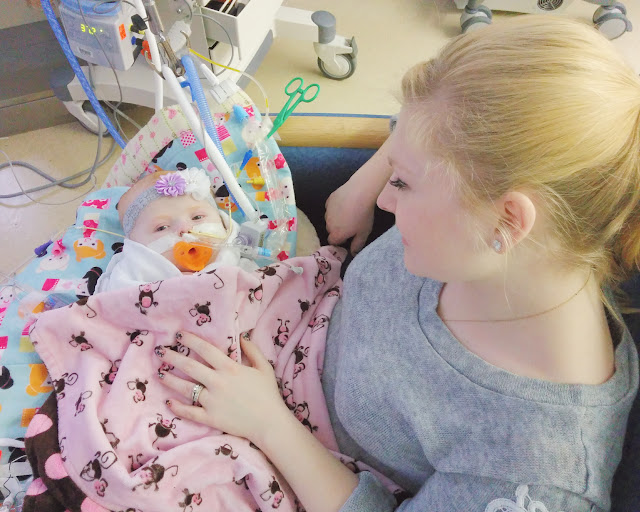
Ava began to smile and stay awake for longer periods of time. She had been on so many sedations for so
long, and every wean just brought out more of her incredible personality. Hope for her future flooded our hearts! We were moved to the TICU (Technology
Dependent ICU) and her recovery only expedited.
Within two weeks, she had weaned off the ventilator for 12 hours at a
time! The TICU team was blown away! We had thought that we would be going home
with nothing more than an empty car-seat, but our Ava fought for us, and I am so proud to say that she proved us
wrong. After 102 of the longest days of
our lives, we were discharged with a positive prognosis in every way. The trach is temporary while she outgrows her
airway trauma, for her lungs get to healthy and strong. We had fought through all of
her drug withdrawal, we managed to keep all 10 fingers AND toes, & lastly, her heart was stable! They told us that other than the need for the
mandatory medications and monitoring, Ava would grow to have no
limitations.
From conception to survival, she is our
miracle.
I have to say a thank you to the family and
community that held us together when we had reached the end of ourselves. When we had no faith, you were our
intercessors. When our emergency funds
became depleted, we not once needed for anything. We could not have made it without the support
of these beautiful people.
It is hard to sum up what CHD means to me.. I
suppose I have to say, it is a reckless love.
I have never known a more reckless, selfless, scary, or beautiful love
since coming to know so many families in the CHD world. The parents, the siblings, the families of
donors have shown us/displayed such a variance of this. Not one of them/us can control our fighter’s
outcome.. and even so, the love is immeasurable.
- Kaila (Ava's mom)