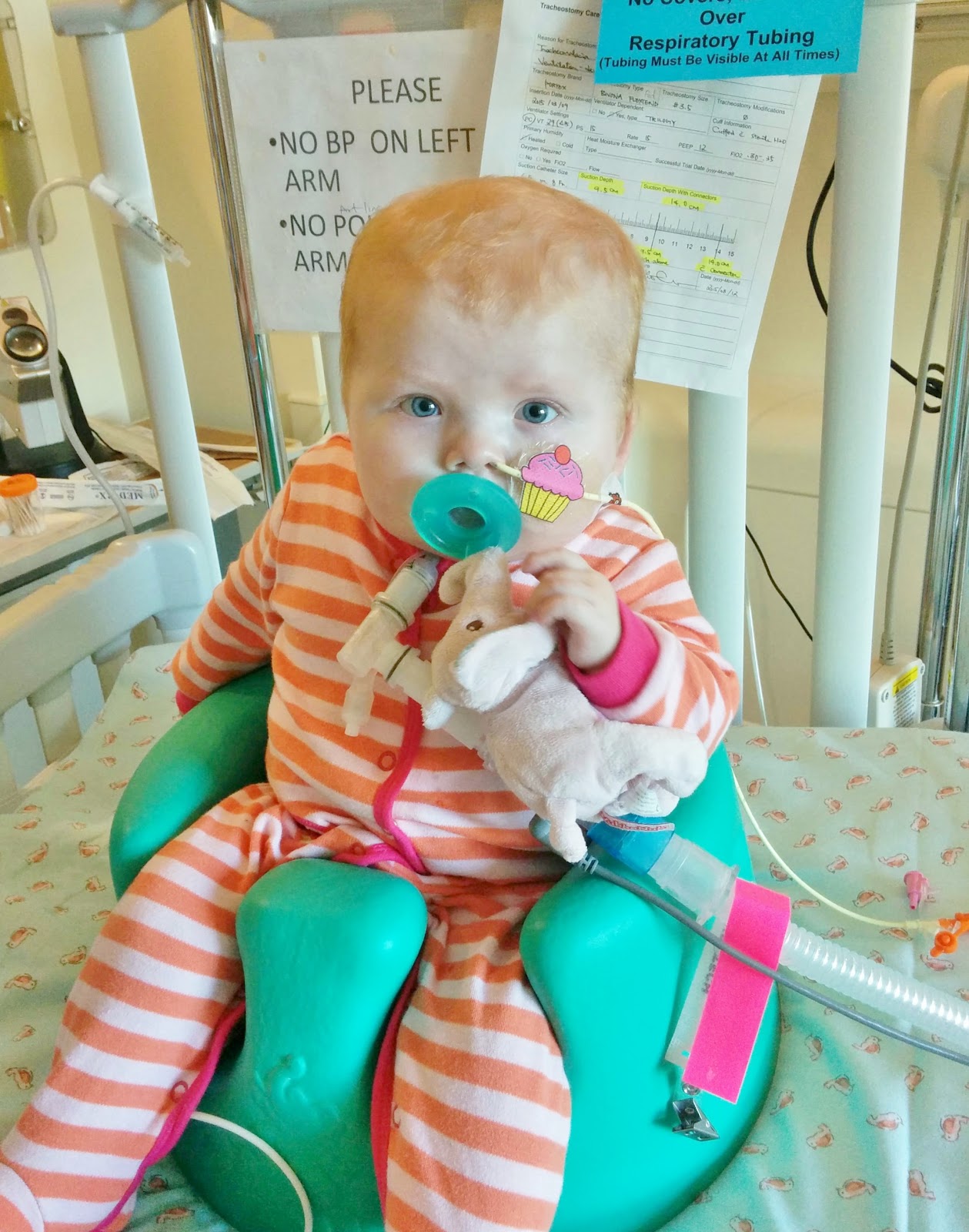
So I know we've been discharged for awhile, and "Home" would probably be a more appropriate title... but I've waited a LONG time to write those words in a blog title!
I swear I’ve
started this blog post several times, but I either don’t save it properly or
had much time to work on it. Then everyday, I get further and further behind
and the task has become somewhat daunting. The last real blog post/medical
update was back at the beginning of September, and we’ve made some major
progress and hit some awesome milestones since then. The biggest is obviously
our DISCHARGE on November 9!! That’s right, we are officially HOME, and this
admission has finally come to an end. We obviously still have a long way to go
in Evanna’s recovery, and unfortunately Evanna has several surgeries and
procedure in her future, but right now, Nick and I are just savouring this
moment and trying to not get caught up when thinking about the future.
I just want
to quickly highlight some of the major milestones that haven’t been documented
here on the blog and relive some of the awesome moments we had. So since that
last real update, Evanna was successfully transitioned from NJ to NG feeding.
For almost an entire year, Evanna has been kept NJ feed for safety purposes
while she was intubated, and then there never seemed to be a right moment to
transition her, as something would happen (infections, surgeries, procedures,
etc) to delay it. Finally once Evanna became line free and completely off
sedation medication (withdrawals didn’t help either….), we were in a good spot
to make the transition. With Evanna we can never do anything quickly, so I set
out a plan to go nice and slow. Well, it did work, but we had to make tweaks
along the way… due to the fact that Evanna was handling the transition well,
but was becoming a “hangry” baby, we did speed up how fast we were increasing
the amount of food we were giving her towards the end. Normally you would
titrate the NJ feeds down while increasing the NG feeds, but for some reason,
Evanna’s tummy doesn’t like 2 tubes going through it, so we had to completely
stop NJ feeds, pull the tube and just feed Evanna through her NG. Overall, it
was a stressful few days, and it was almost as painful as watching a baby go
through withdrawals, but all was well once we reached full feeds and Evanna was
able to rest comfortably (it’s moments like this where I wish you could reason
with a baby lol).



The first
week of October was a busy one for us. First I held a little party to celebrate
#EvannasHeartHospitalversary. Many heart families celebrate the anniversary of
their child’s first open heart surgery, but because we were still hospital, I
felt it was important to celebrate BOTH milestones. It’s not very common for a
child to spend an ENTIRE year in hospital (it does happen, but again, it’s not
something you hear about everyday), so not only did I want to celebrate the one-year
mark since Evanna’s first major OHS, but also our journey and everything that
our family went through. It had been an incredibly hard year for Nick and I,
and while it could have easily broken us, it only made our bond stronger. While
I was proud of how well Nick and I endured, the night before October 6 was incredibly
emotional for me. Our first year as family should have been spent making fun
memories, but instead it was spent by our child’s bedside while she recovered
from surgery after surgery and complication after complication. There were days
that I hated social media, because while my friends were enjoying the holidays
and family traditions, Evanna was intubated and fighting for her life. At times
I hated “how unfair” our life was and was very angry at our predicament, but
thankfully those moments were few and far in between. As weird as it sounds, I
needed to celebrate this milestone, otherwise I might have done the opposite. I had a special crown made for Evanna, invited
our close friends and family, and arranged for a special cake to be made
through an organization called Icing Smiles (blog post to come). It was a great
afternoon, and it was great to see some people that I hadn’t seen in a very
long time.


A few days
after the party, Evanna finally went
for a little trip back to the ICU for a trach transition. When we initially
came out of ICU, they told us that out biggest hurdle towards taking Evanna
home was the fact that Evanna had a cuffed trach. They really don’t like to
send kids with cuffed trach’s home (not impossible, but something they like to
avoid if at all possible), so it was decided that once Evanna was stable and
spent a month out of ICU that we would try and switch Evanna to a cuffless
trach and see how she would handle it. Well, we tried to do it at the end of
September, but due to a bed shortage in the ICU and then Evanna’s party, it got
held off until October 5. I often get people telling me that things will happen
when they’re suppose too, and more often than not, it ends up being true. On
the eve of October 6 (our Heartiversary), and on Day 365 in hospital, we took
Evanna back down to the ICU and try to transition Evanna to a cuffless trach.
We originally planned to spend at least 24 hours in the ICU to give the RT’s
some time to fiddle with her settings, but within 6 hours of the trach change
and no fiddling required, the intensivist stated that Evanna was doing just
fine and didn’t really need to be in the ICU any longer. So once the resident
completed the paperwork, Evanna was taken back up to Unit 2 later that night,
and all was well.



After
Evanna’s trach transition, we had a big meeting with her medical team to
discuss where to go from here. Just before Evanna transitioned out of the ICU
at the end of August, we had this huge transfer meeting, and it was discussed
that Evanna would most likely not be discharged until closer to Christmas, and
even that wasn’t a guarantee. However, due to how well the trach change went
and how uneventful the whole process was, it was decided that maybe Evanna was
ready to go home. Yes, there were still some small issues, but none that were
big enough to keep us in hospital anymore, and so it was time to really work
towards discharge. When it came time to pick a time frame, they asked for our
opinion, and I asked if mid to late November was appropriate, to which they
responded with yes. You see, with a trach (and vented) baby, discharging for
the first time is not a quick process – Nick and I needed to make sure we were
fully trained to take care of her, we had to proper equipment in our home, and
have staff (who were also properly trained) in place to watch and take care of
her at night time. This we were told would be our next biggest hurdle, but I
was not about to let that stop us from bringing Evanna home. Over the past
year, Evanna has garnered a little bit of an audience that just absolutely
adores her and so I decided to use that attention to help us find nurses! Nick
and I decided to do “self managed care”, which is an option here in Alberta
that puts me and Nick in charge of who takes care of our daughter (yup – that’s
right, we essentially are bosses, hire and train whomever we want), but are
funded through Alberta Health Services (which means based on Evanna’s needs, we’re
given a certain amount to pay for night nursing plus a little extra for day
respite care). So I put an ad up on the internet, and pleaded for people to
spread the word and share that we were looking for nurses – and it actually
worked! Within a day, I had several resumes in my inbox, and by the end of the
week, I roughly had 50 great resumes of people wanting to care for our little
girl. It was actually a little overwhelming, and became an emotional process…
over the past year, Nick and I felt like we only experienced setback after
setback, and for once things seemed to being moving forward at a quicker rate
and without any hiccups (so yes I cried, but because I was so happy and was
feeling so blessed). A one-point Nick even asked me if this was really
happening and if I thought Evanna was actually going to come home this time –
to which I smiled and said “yes”. There were times where we would avoid using
certain words like “home” and “discharge”, as we felt it always jinxed the
situation, but I was so confident that “this was it”, that I used those words
with confidence.
Now don’t
get me wrong, the last few weeks before our tentative discharge date were
filled with mini hurdles and a todo list that was a mile long, but we didn’t let that
stop us, and we hit the ground running. We both got our CPR done (Nick needed to get re-certified for work anyways, so it was like killing two birds with one stone), our trach
training completed (trach changes, suctioning, bagging, etc), NG/food pump training,
vendors in place (fun fact that I haven’t been too public with on Evanna's FB page or my IG account – but my Uncle
actually owns a large oxygen vendor company here in Alberta… so lets just say
that he has made sure we’ve been well taken care of and a great support to
our family through this entire journey/process. It’s been surreal that a company
I grew up with is now in my HOME keeping my child alive!), staff hired and
trained. Our timeline of mid to late November was actually pushed UP to the
beginning of November, and I was getting my birthday wish of having my daughter
home! We began to get more and more freedom within the hospital (even taking
Evanna on unaccompanied walks around the hospital was a big deal in the
beginning) and we even began to plan day passes to take Evanna out of the
hospital and have a few quick trips home.





Now it just
wouldn’t be right if we didn’t experience any hiccups towards the end, even up
until the last weekend in hospital, and we unfortunately had to put up a small
fight and convince Evanna’s medical team that not only was Evanna ready to come
home, but that Nick and I were more
than capable of handling her and had the proper experience and knowledge to
take care of her. In both the discharge meeting and several side conversations,
it was reiterated several times to us that Evanna is one of the more complex
cases that has come their way in recent years (complex heart + complex airway =
complex mess), and her safety was super important to them. While we were
grateful for their concerns, and that they truly cared for our daughter, Nick
and I began to see the hospital as a detrimental place and was beginning to
hinder her progress. The biggest issue we had was with certain people not responding
to Evanna appropriately when she was upset. When a trach and vented baby
desats, they have a certain protocol that they follow to bring that child out
of that desat – however, Evanna being first and foremost a CARDIAC baby, those
rules for the most part do not apply, and if anything, it can make her angrier,
desat further and take a longer time to recover. They began to discuss these as
“episodes” or “events”, but funny thing was they never happened when Nick or I
were there, and it was because when something was making Evanna angry, we were
there to catch it, deal with it quickly, and in the appropriate manner.
Whenever Evanna is having a desat, Nick and I know exactly what to do and never
make a big deal out of it (ie. tell the nurse or make the medical team aware) because
like with many cardiac babies, the best way to handle it is to calm the child
down and support them through the “event”. Anyways, it became this whole
ordeal, and it was frustrating because we couldn’t be there all the time and
handle Evanna’s “episodes”. **I would like to clarify that it sounds a lot
worse than it really is. Evanna is just being like any other heart baby with a
VSD – when she gets mad or angry, cries and doesn’t take nice deep breaths, her
heart will shunt, which means her oxygenated and deoxygenated blood mixes more
than usual, and the deoxygenated blood gets circulated throughout her body.
Then you bring a stranger into the situation who doesn’t know Evanna’s likes
and dislikes, and can make her even angrier, and therefore a longer and more
severe desat. Overall, Evanna is just unique in that she has lower oxygen
saturations to begin with, is hooked up to a monitor, and so when she’s angry,
her numbers can freak people out. It’s hard for some people to wrap their head
around the fact that when trying to get Evanna’s numbers to come back up, they
can’t treat her like a respiratory baby (which you can PHYSICALLY see with her
trach and vent), but must treat her like a cardiac baby (which you can’t really
see on outside as it’s less obvious). At the end of the day, we knew it was
time to get Evanna home, because the hospital wasn’t the safest place for her
anymore, and that things were beginning to shift and our home would be a safer
place for her under our watchful eyes of people who truly knew Evanna best.



Finally, on November
9, we packed up Evanna’s final belongings and walked out those hospital doors!
Well, technically we made a stop in the PICU, as when we transferred out of the
ICU back in August, they asked if we could stop by before we actually went home
on discharge day. Evanna spent a total of 13 months in hospital, but 11 of
those months was spent between the Stollery and ACH’s PICU’s, and so we had
built some major relationships with the staff between those two units. The
timing was actually quite perfect – Dr. Mahoney happened to be working! She was
the intensivist who pretty much saved Evanna’s life on Canada Day when she went
into Septic Shock, and both Nick and I felt that it was perfect that she got to
be the one to see us off, and be the final “medical” person that we saw before
we walked out of those doors.
So, what
have we been up too since we’ve been home? Well for the most part we’ve been
trying to just catch our breath, work out the kinks, find a system, and get into a
grove. After a year of our life being put on hold, we’re just trying to regain
some normalcy and pick up where we left off. So what does that mean? Well, I’m
actually to returning to work after Christmas part-time, but made it
so I only work around Nick’s schedule. We also bought and are in the process of
building a new house! While the timing hasn’t been the best (the day we got a
quicker discharge date for Evanna, happened to be the same day we put on a hold
on the lot), but if we didn’t act when we did, we would have lost out on
this particular opportunity. We’ve actually been looking for a new house since
Evanna transferred back to Calgary at the end of June, and I was hoping to move
before Evanna came home, but nothing we found was within our price range nor
had what we were looking for. At one point did find a great property with
potential, but it sold before we even got a chance to look at it and I was so
bummed out, however, turns out that an even better house was waiting for us, and
I saw that things were working out the way they’re suppose too. Anyways, we don’t
get possession until late summer, so other than attending a few house
appointments here and there (like picking out floors and cupboards), it’s not
really on our radar, as we have other things that consuming our attention right now.
Ahh – feels
so good to be caught up! I have a few blog posts planned (ie. Evanna’s New “Nursery”
Reveal, Icing Smiles, etc), and a few blogging projects I wanted to get done,
but I felt I couldn’t commit to anything until I was at least caught up here.
Thanks for
reading, following along and keeping our little family in your thoughts and
prayers!
xo The
Irvine Family